Treatments for Bladder Cancer have gotten a lot better over the past few decades, which means that more people are living longer after surgery or medicine. This has led to a new area of Bladder Cancer care called “survivorship,” which looks at the patient’s health as a whole and sometimes uses treatments that haven’t always been in the oncology playbook.
[powerkit_toc title=”Table of Contents” depth=”2″ min_count=”4″ min_characters=”1000″ btn_hide=”true” default_state=”expanded”]
In the case of bladder cancer, living longer and having a better quality of life after surgery can be helped by physical therapy that focuses on making the pelvic floor work better. Dr. Matthew Mossanen, a surgical oncologist at Dana-Farber Bladder Cancer Institute in Boston and an assistant a Harvard Medical School professor of surgery says that the muscles in the pelvic floor keep the bowels and bladder healthy and working.
Health Clinical Specialist In New York City
Ting-Ting Kuo, a board certified women’s health clinical specialist and director of rehabilitation at In New York City, the Memorial Sloan Kettering Cancer Center says that the bowl-shaped structure at the base of the pelvis is made up of a group of muscles, ligaments, and connective tissue.

Having the right muscle tone and control in this area helps with core stability, bowel function, urinary control, and gives support to other organs.
Read Also: A Global Revolution by Ludwig Guttman: The Paralympic Movement
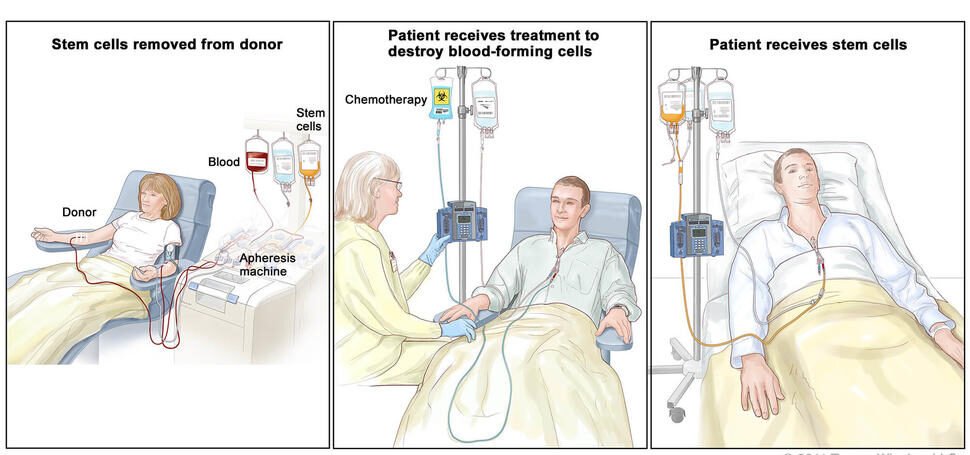
Chemotherapy
Bladder cancer treatment can be invasive and mess with these structures and functions. Even though statistics show that chemotherapy followed by surgery is usually the best way to stay alive for a long time, this surgery can change how this part of the body works. Some people with bladder cancer have a cystectomy, which is a major surgery that “involves removing the bladder and, in men, removing the prostate,” says Mossanen. “It means taking out the uterus, ovaries, fallopian tubes, and part of the vagina for women. It’s a big surgery that’s done when bladder cancer is so bad that it could kill the person.

Dr. Emily Slopnick, an urologist at the Cleveland Clinic in Ohio, says that most people with bladder cancer don’t have to have a cystectomy. This surgery is only for people with advanced bladder cancer who are young enough and healthy enough to go through such a difficult procedure. After it’s taken out, the urinary system will need to be fixed, since the kidneys will still make urine that needs to go somewhere. Mossanen says that this is mostly done in one of two ways.
How to do Chemotherapy?
The first option is a urostomy, in which a surgeon makes an opening in the abdomen through which urine can flow into an external bag that can be emptied when it gets full. Neobladder is the second main option. This means making a new bladder inside the body. “A neobladder is a replacement bladder made from a piece of intestine,” says Mossanen. Mossanen says that making a neobladder “can give patients a very good quality of life” by letting some younger people avoid using a bag. Slopnick says that all of these changes to the urinary system can lead to problems. “Any kind of damage to the pelvis can cause the pelvic floor to react.
The pelvic floor muscles tighten as the body tries to protect itself from the trauma. often tighten up or spasm. This can make it hard to stay dry, have a sexual life, or go to the bathroom. Also, especially after a neobladder reconstruction, some patients may develop a number of unwanted symptoms, such as urinary incontinence, an inability to fully empty the bladder, and urine leakage, especially when laughing, coughing, or sneezing. But Mossanen says that sending patients with these problems to a pelvic floor physical therapist can help because rehabilitating these important structures may help bladder cancer survivors live a better life.
How to Use It Physical Therapy Of Bladder Cancer?
Physical therapy is usually thought of as something that is done after surgery to help restore that has been lost because of illness or surgery. However, in the case of bladder cancer, Mosinee says that rehabilitation of the pelvic floor may also be a good idea. He says, “I really do believe in prehab with all my heart.” Mossanen has made programs like this at the Dana-Farber Bladder Cancer Institute to help people get ready for surgery. As part of these efforts, patients can take classes on health in general, nutrition, and exercises that can help them get stronger before surgery. The idea of prehab makes sense: if you’re stronger before surgery, you’ll probably heal faster.

Mossanen thinks that prehab will likely become a more common part of bladder cancer treatment in the future, even though the idea hasn’t caught on everywhere just yet. Prehab can be especially helpful for people getting ready for a cystectomy and the long time it takes to heal after surgery (about three months). “Many patients feel tired after surgery and have a slow recovery or other problems,” says Mossanen. In some cases, this is because chemotherapy is often given before a cystectomy. “Because of these things, some patients can’t take part in rehabilitation. This is a great reason to do prehab so that patients can get better faster.”
Why Patient Need of Pelvic-Floor Prehab or Rehab?
Whether you need pelvic-floor prehab or rehab because of bladder cancer, you will work with a pelvic floor specialist. This is usually a pelvic floor physical therapist or a physiatrist, a doctor who specializes in rehabilitative medicine. These experts are trained and know how to help you get your function back and avoid problems.
Kuo says that when and how that provider gets involved depends on the symptoms and the type of care being given. “A multidisciplinary team will decide when a person with bladder cancer should be sent for pelvic floor therapy.”
What To Expect Physical Therapy After Bladder Cancer
Slopnick says that if you have bladder cancer and will be getting physical therapy, you can expect a very thorough physical exam. “They’ll figure out what you’re good at and what you’re not.” This could be done by putting a probe in the vaginal canal or rectum and watching how the muscles move on a screen. The therapist will also check your hips, spine, back, and abdominal muscles to see how strong they are and how well they work together. Your medical history will be carefully thought about as your personalized care plan is made. For example, if you have to go to the bathroom more often or feel like you have to go more often after surgery, these changes may help the pelvic floor specialist figure out what to work on during therapy.
Cancer hasn’t stopped. Contact your GP if you have:
Blood in your wee
Frequent need to wee
↩️ Recurring UTIs
If you have cancer, you will get checked & treated. The NHS will give you the care you need.
#CancerAware#BladderCancer pic.twitter.com/2kYjylLF24
— Fight Bladder Cancer (@BladderCancerUK) August 10, 2022
During this first evaluation, the therapist will take measurements of how well the pelvic floor is working. They can check these measurements again over time to see how well the therapy is working and if there is a need to change the care plan. Slopnick says that when it comes to the therapy itself, it’s always best to work with a trained provider. “I wouldn’t just read about it online and try to figure it out on your own, because you’ve been through a complicated disease and some complicated treatments. Find out what’s wrong by going to the doctor if it’s just the pelvic floor and to make sure nothing else is wrong.”
Read Also: Healthy Living | Your Roadmap to Wellness
How Long Pelvic Floor Therapy Works?
It’s hard to say how long pelvic floor therapy will last because it depends so much on the person’s needs and physical condition. But, Kuo says, “to start, it’s usually once or twice a week.” She says that some patients may need to do exercises at home as well as in therapy. “The most important thing is that each person gets the same care every time.”
Possible treatments include breathing exercises, exercises to build strength or relax, and massage to loosen up tight muscles. In other words, you can’t just do Kegels and be done with it. “And it’s not just the muscles around the pelvic girdle. Your legs, your trunk, your abdomen, your core, and your back are all involved. We look at how well the muscles work together and make sure that everyone has good mobility,” Kuo says. During this therapy, you may even do exercises to improve your posture and the way you sit or stand.
Rehabilitating The Pelvic Floor Can Help Bladder Cancer Patients in Many Ways:
As the therapy goes on, “we’ll look at some objective measures of the strength and coordination of the pelvic floor muscles,” Kuo says. This can include checking the flexibility and mobility of soft tissues, the amount of scar tissue, and the number of symptoms. “We check to see if [patients] cut down on the number of incontinence pads they use or lengthened the time they can go without going to the bathroom.”
Mossanen adds that for some patients, the psychological benefit of working closely with a physical therapist to improve pelvic floor health may be more important than these improved measurements. As a surgeon, he says, “I think it’s good for the patient’s mind and heart to have support from another team member who can offer something I can’t.”
How to Get Back To Normal After Having Your Bladder Removed By Surgery?
Other Steps Were Taken
In addition to physical therapy, nutritional counselling is often a part of recovery from bladder cancer. Bowel function is a concern, especially for people who have a neobladder made from a piece of intestines. “That’s the most important thing we’re looking for after surgery: for the bowel function to come back,” says Slopnick. “As the bowels heal from surgery, they slow down,” she says. Patients are usually told not to eat too much fiber and to drink a lot of water during this time to help the gut heal and do its job.
Kuo also says that people who have had a neobladder procedure should drink a lot of water. This is because the new bladder pouch is made from a piece of intestinal tissue, which doesn’t have the same nerve endings or muscles that the urinary bladder did. With the neobladder, the feeling of having to go to the bathroom quickly can be very different. “They won’t have the muscle in their bladder to tell them when they need to go, so they might need to set a time every few hours to go,” she says. Gentle exercise, like getting up and walking as soon as possible after surgery, can help keep the digestive system moving and stop problems like blood clots from happening.
Surgery for Bladder Cancer
When getting surgery for bladder cancer, there’s a lot to know, and some of it might make you feel a little weird. It can be awkward to talk to anyone, let alone a room full of doctors, about how your bowels and bladder work and what you do in the bathroom. But you can get help from other people. “Talk to your doctor if you have any symptoms,” Kuo says.



